By Dr Gerard Ee
Acne is not a hygiene problem. It is a chronic inflammatory disorder of the pilosebaceous unit. When inflammation recurs month after month, the natural history of the disease results in post acne erythema, post inflammatory hyperpigmentation and this can sometimes even lead to permanent scarring.
My view on acne treatment Singapore is straightforward. The therapeutic aim is to reduce sebaceous gland activity, normalise follicular keratinisation, reduce the burden of Cutibacterium acnes and suppress the inflammatory cascade. [1,2,3]
Acne develops through several biological pathways at once. The oil gland and hair follicle complex becomes obstructed, resulting in sebum output rising C. acnes proliferates within the plugged follicle. Inflammation then amplifies the lesion and often begins before the papule is visible on the surface. This is why random spot treatment and frequent product changes rarely work. Acne is not a one product disease, so it rarely responds to a single product trying to cure the acne. [1,2]
This is the clinical mistake I see most often. Patients telling me, they are only on Differin. That’s it. It never works. Patients treat active inflammatory acne as though it were only excess surface oil or a temporary breakout. By the time they seek proper care, they are no longer treating acne alone. They are managing persistent erythema, pigment change, textural injury and scar risk. Effective acne treatment Singapore depends on early control, not delayed rescue. [1,3]

Acne requires a biological treatment strategy
In clinical practice, acne management should be built on biology and a good understanding of physiology. A useful treatment plan must do four things. It must keep follicles open. It must reduce excess sebum. It must control the microbial environment within the follicle. It must reduce inflammation before tissue damage accumulates. This is why rational combination therapy remains the backbone of acne care. [1,3]
For mild comedonal acne, a topical retinoid remains the foundation. Retinoids correct abnormal keratinisation and reduce microcomedone formation. Benzoyl peroxide is added when inflammatory lesions are present because it reduces bacterial load and has direct anti- inflammatory activity. Azelaic acid is valuable when acne coexists with pigment change, sensitive skin, or both. Topical antibiotics can help selected patients, but they should not be used as prolonged stand-alone therapy because resistance is a predictable consequence. [1,3]
For moderate inflammatory acne, treatment usually needs more than surface care. Oral antibiotics still have a role, but their role is limited. They are a temporary anti-inflammatory bridge. They are not a long-term maintenance plan. In my view, repeated antibiotic courses without a clear exit strategy reflect weak acne management. Once inflammatory control has been achieved, maintenance must shift to a regimen that prevents new lesion formation rather than simply suppressing flares after they appear. [1,3]
For nodular, cystic, scar prone, or refractory acne, isotretinoin remains the most decisive medical therapy. It is the treatment that most directly reduces sebaceous gland function and changes the long-term trajectory of severe acne. The key clinical error is waiting too long. If scars are accumulating, a prolonged sequence of half measures is often more damaging than timely escalation. [1,2,3]
Hormonal acne follows a recognisable pattern
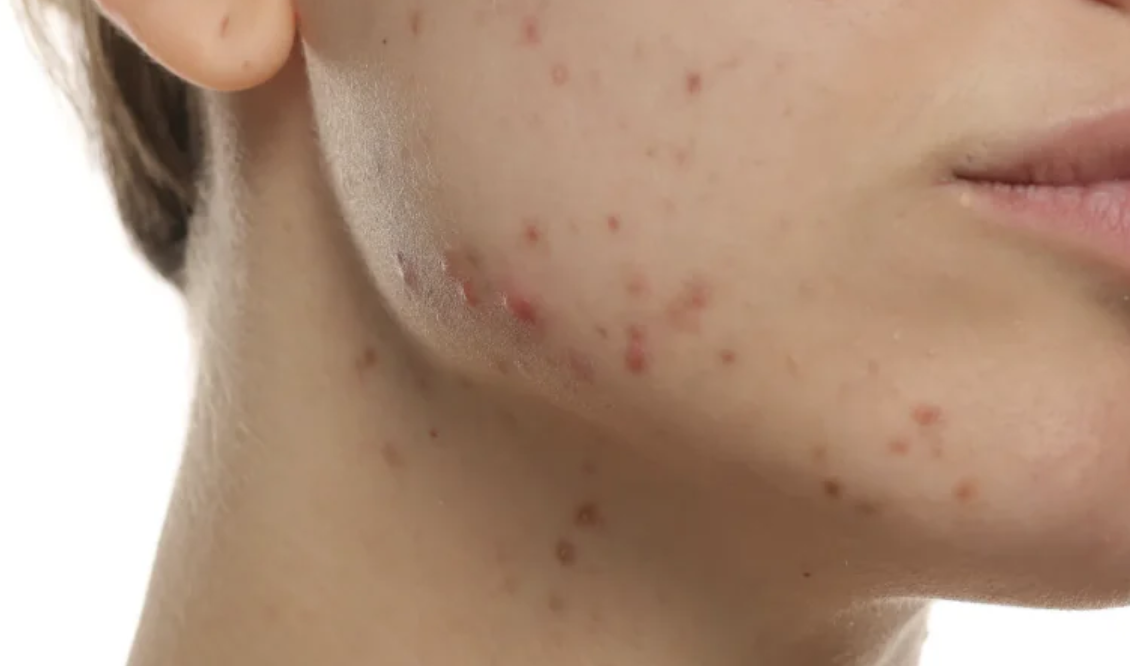
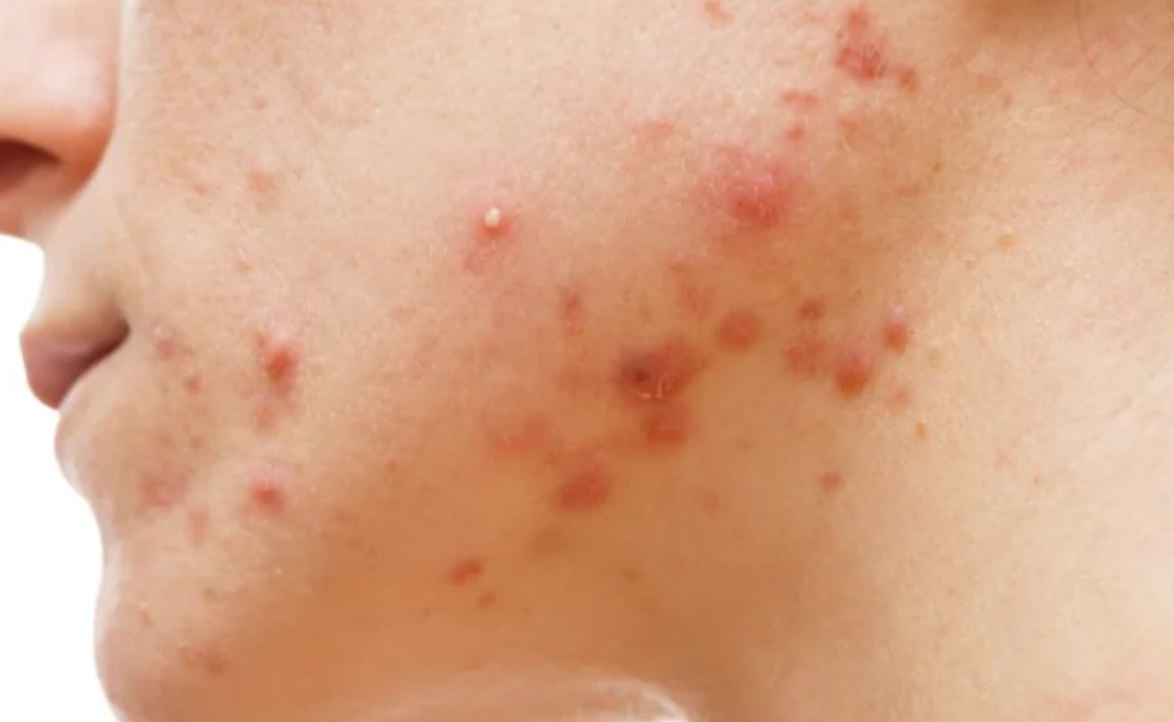
Hormonal acne treatment should be guided by pattern recognition rather than assumption. Hormonal acne is driven by androgen activity within the pilosebaceous unit. It is especially relevant in adult women and often presents as inflammatory lesions over the chin, jawline and lower face. These lesions are often deeper, more persistent and more likely to recur. [1,3,5]
Three adult female acne patterns are recognised. Persistent acne continues from adolescence into adult life. Adult-onset acne begins for the first time in adulthood. Recurrent acne returns after a period of remission. These patterns matter because they influence how strongly androgen signalling should be considered in the treatment plan. [1,5]
The purpose of hormonal acne treatment is not to label every adult female breakout as endocrine disease. The purpose is to identify the subgroup in which androgen activity is a major driver. The clinical clues are familiar. Lower face inflammatory acne is one. Menstrual flares are another. Irregular cycles, hirsutism, androgenic alopecia, sudden severe onset and rapid relapse after isotretinoin are more important warning signs because they raise the probability of androgen excess. [4,5]
Not every woman with acne needs a hormone panel. Testing should be selective. It becomes more relevant when acne coexists with clinical hyperandrogenism, when standard therapy fails without a clear reason or when the onset and severity are out of keeping with routine acne. In most cases the endocrine concern is polycystic ovary syndrome rather than a rare tumour, but good clinical judgement still matters. [4,5]
Hormonal acne treatment needs the right therapeutic target
When androgen signalling is central to the disease pattern, hormonal acne treatment becomes more rational than yet another course of antibiotics. Combined oral contraceptives reduce ovarian androgen drive. Spironolactone blocks androgen receptor activity and reduces the sebaceous response to circulating androgens. These are not cosmetic add-ons. They are biologically targeted interventions for the right patient. [3,5]
This is an important point in modern acne treatment in Singapore. Many adult women with recurrent jawline acne are treated for too long with surface products alone. That approach fails because the dominant biological driver has not been addressed. In women with menstrual flares, persistent lower face inflammation, or clear features of androgen excess, hormonal therapy often makes more sense than repeated antimicrobial suppression. [3,5]
Response to hormonal therapy requires patience. Combined oral contraceptives and spironolactone do not behave like rescue medication. Their benefit builds over time. A full therapeutic judgment usually requires several months. That timeline should be explained early, because premature switching is one of the common reasons good treatment is abandoned before it has had a proper chance to work. [3,5]
Pregnancy risk and medical suitability must also be considered carefully. Spironolactone is not suitable in pregnancy. Combined oral contraceptives are not suitable for every patient. This is why hormonal acne treatment should be individualised rather than standardised. The correct therapy is the one that matches both the biology of the acne and the safety profile of the patient. [4,5]
Clascoterone has expanded topical hormonal acne treatment
One of the most important additions to acne therapeutics is Winlevi, of which the active ingredient is Clascoterone. Clascoterone is a topical androgen receptor inhibitor. It acts directly within the skin and provides a local antiandrogen approach without relying entirely on systemic hormone manipulation. This is a meaningful development because it expands the treatment options for androgen-responsive acne. [6]
In two phase 3 randomised clinical trials, Clascoterone cream produced significant improvements in both inflammatory and non-inflammatory lesions compared with vehicle, with a favourable safety profile. From a clinical standpoint, putting on Winlevi / Clascoterone is especially interesting for patients with mild to moderate acne in whom androgen signalling appears relevant, but who are not ideal candidates for oral hormonal therapy or who prefer a topical route. [6]
This does not make Winlevi for acne a replacement for all other treatments. It is best viewed as an additional tool. In the right patient, it fits naturally into a rational hormonal acne treatment plan. In the wrong patient, it will still underperform if the acne is severe, deeply nodular, or already scar-driven. Good treatment depends on patient selection, not product enthusiasm. [3,6]
AviClear has created a new category of sebaceous gland-targeted treatment

AviClear deserves serious attention because it is based on a clear biological target. It is a 1726 nm laser designed to achieve selective photothermolysis of sebaceous glands by targeting sebum-rich structures. That wavelength matters because it allows focused sebaceous gland injury while preserving surrounding skin through effective epidermal cooling. [7,8]
This is not simply another light-based acne device. The concept is more precise. It addresses one of the central engines of acne pathogenesis, which is sebaceous gland overactivity. From a mechanistic point of view, that makes AviClear particularly relevant for inflammatory acne that is clearly sebum-driven. [7,8]
The clinical data are also important. Prospective studies have shown progressive reduction in inflammatory lesions after a standard series of three treatments. Improvement continues well beyond the treatment window. Reported one-year outcomes show durable benefit across skin types, with a high proportion of patients reaching at least a fifty per cent reduction in inflammatory lesion counts. A substantial proportion becomes clear or almost clear by long-term follow-up. [9,10]
Safety has also been encouraging. The treatment has been well-tolerated across different skin types. Transient erythema and oedema are the most common short-term effects. Pigmentary complications have not been a dominant signal in the published prospective studies. [7,9,10]
My view is that AviClear has a defined place in acne treatment Singapore. It is most compelling in patients with persistent inflammatory acne who want a drug-sparing strategy, who are unsuitable for systemic medication, or who prefer a sebaceous gland-targeted approach.
It is not the answer to every acne phenotype. Severe nodulocystic acne may still need isotretinoin. Clear endocrine patterns may still need hormonal acne treatment. Device-based therapy is strongest when it is chosen for the right biology. [3,7,8,9,10]
AGNES RF is a precision tool for selected patients
AGNES RF belongs to the broader category of sebaceous gland-targeted radiofrequency microneedling. Its logic is different from laser treatment. Instead of using a wavelength that is selectively absorbed by sebum, it uses insulated microneedles to deliver radiofrequency energy into the deep dermis and create selective electrothermolysis of sebaceous structures. [11,12,13]
This makes AGNES RF especially relevant for localised inflammatory lesions, recurrent nodules and patients in whom focal sebaceous gland activity is the dominant problem. In my view, its strength lies in precision. It is a highly useful tool when the disease pattern is focal and deep. It is less persuasive when the acne is diffuse, hormonally driven, or severe enough to require systemic control. [11,12,13]
The evidence base supports this selective role. A prospective randomised controlled study showed a significant reduction in inflammatory lesions by twelve weeks when a single microneedle radiofrequency device was used to target sebaceous glands. Other radiofrequency studies have shown reductions in inflammatory lesion counts, lower sebum excretion and sustained improvement for up to one year.
Comparative work has also suggested that microneedling radiofrequency can perform well against other device-based acne treatments, with favourable patient satisfaction in selected settings. [11,12,13,14,15]
AGNES RF should therefore be seen as a precision option within a wider treatment ladder. It is not a universal replacement for topical therapy, isotretinoin, or hormonal acne treatment. It is most useful when the clinical pattern justifies focal sebaceous gland targeting and when treatment is performed by an experienced operator. [12,13,14,15]
Device-based treatment should complement good clinical judgement
Modern device-based acne therapy is evolving quickly. Laser and light-based treatments are becoming more sophisticated because they now target relevant biology rather than relying on nonspecific heat alone. That progress is real. It deserves attention. It also needs discipline. [8,16,17]
In my clinical view, the question is never whether a device is fashionable. The question is whether the device matches the acne pattern. AviClear is more attractive when sebaceous overactivity and diffuse inflammatory acne dominate. AGNES RF is more attractive when focal deeper lesions dominate. Neither should be used as a shortcut around proper diagnosis. Neither should distract from the need to recognise severe acne early, identify endocrine clues and escalate when scar risk is rising. [8,16,17]
Timelines matter in acne treatment in Singapore

Patients often judge treatment too early. That creates frustration and poor adherence. A biologically sound acne regimen needs time. Topical retinoids need several weeks before their comedolytic benefit becomes fully visible. Oral antibiotics are temporary anti-inflammatory tools, not overnight solutions. Hormonal acne treatment usually needs three to six months for a fair assessment. Isotretinoin is a course based treatment, not a short intervention. AviClear continues to improve beyond the final session. AGNES RF also needs follow-up because lesion reduction and sebaceous changes evolve over time. [3,5,9,10,12,14,15]
This is why adherence matters as much as intensity. A good plan followed consistently will outperform an excellent plan used for only two weeks. The best acne treatment Singapore strategy is biologically rational, appropriately timed and sustained long enough to change the course of the disease. [1,3]
The practical hierarchy I use in acne treatment in Singapore
My treatment hierarchy is simple. If the acne is primarily comedonal, I build around a retinoid-based topical regimen. If it is inflammatory but not severe, I use a combination of topical therapy and a time-limited oral anti-inflammatory bridge when necessary. If the pattern is clearly androgen-driven, I move earlier toward hormonal acne treatment.
If the disease is nodular, scarring, or refractory, I escalate decisively toward isotretinoin. If the patient needs a drug-sparing strategy or has a pattern well suited to sebaceous gland targeting, I discuss AviClear or selected radiofrequency options. [1,3,5,7,12]
The unifying principle is straightforward. Treat the biology that is actually present. Do not undertreat scar-prone inflammation. Do not overcomplicate mild acne. Do not use devices as decoration around an untreated endocrine problem. When the diagnosis is correct and the pathway is matched to the patient, outcomes improve. [1,3,4]
FAQ About Acne Treatment Singapore
What is the best acne treatment Singapore option?
There is no single best option for every patient. The correct treatment depends on the dominant biology of the acne. Comedonal acne, inflammatory acne, hormonal acne, nodular acne, and scar-prone acne do not belong on the same treatment pathway. [1,3]
When is hormonal acne treatment appropriate?
Hormonal acne treatment is most appropriate when acne is persistent, lower face dominant, linked to menstrual flares, or associated with signs of androgen excess such as irregular cycles, hirsutism, or androgenic alopecia. [4,5]
Is hormonal acne always caused by PCOS?
No. PCOS is a common association, but it is not the only explanation. Hormonal acne reflects androgen activity at the pilosebaceous unit. Some patients have clear endocrine features. Others have acne that is hormonally patterned without a major underlying endocrine disorder. [4,5]
Should every adult woman with acne have hormone tests?
No. Hormone testing should be selective. It is most useful when acne is severe, sudden in onset, resistant to standard treatment, or accompanied by clinical hyperandrogenism. [4]
Is AviClear better than isotretinoin?
They address different clinical situations. Isotretinoin remains the most decisive therapy for severe, nodular, or scar-prone acne. AviClear is a strong option when sebaceous overactivity is central and a non systemic approach is preferred. [3,7,9,10]
Is AGNES RF useful for cystic acne?
It can be useful when cystic or nodular lesions are localised and recurrent. Its strength lies in focal sebaceous gland targeting. It is less suitable as a stand alone answer for diffuse severe acne. [12,13,14,15]
Can topical clascoterone replace oral hormonal therapy?
In selected patients with mild to moderate androgen responsive acne, it can provide a valuable topical antiandrogen route. In deeper, more persistent, or more severe hormonal acne, systemic therapy may still be more appropriate. [5,6]
How early should acne be treated?
As early as possible once inflammatory acne is recurring or scars are beginning to form. Early control reduces the risk of long term pigment change and permanent textural injury. [1,2,3]
Conclusion
Acne is a chronic inflammatory disease with a predictable biology. It is not well managed by random product rotation or by treating each breakout as an isolated event.
My view on acne treatment Singapore is clear. Treatment should be mechanism based. It should reduce sebaceous gland activity, correct follicular obstruction, control C. acnes, and suppress inflammation before scars appear.
Hormonal acne treatment should be used when the clinical pattern points to androgen driven disease. AviClear and AGNES RF both have a legitimate place in modern acne care, but only when they are matched to the right patient. Good outcomes come from precision, timing, and a willingness to escalate before damage becomes permanent. [1,3,5,7,12,16,17]
References
- Zaenglein AL. Acne Vulgaris. The New England Journal of Medicine. 2018.
Hyperlink: https://doi.org/10.1056/NEJMcp1702493
- James WD. Acne. The New England Journal of Medicine. 2005.
https://doi.org/10.1056/NEJMcp033487
- Eichenfield DZ, Sprague J, Eichenfield LF. Management of Acne Vulgaris: A Review. JAMA. 2021.
https://jamanetwork.com/journals/jama/article-abstract/2786495
- Elhassan YS, Hawley JM, Cussen L, et al. Society for Endocrinology Clinical Practice Guideline for the Evaluation of Androgen Excess in Women. Clinical Endocrinology. 2025.
https://doi.org/10.1111/cen.15265
- Barros B, Thiboutot D. Hormonal Therapies for Acne. Clinics in Dermatology. 2017.
https://doi.org/10.1016/j.clindermatol.2016.10.009
- Hebert A, Thiboutot D, Stein Gold L, et al. Efficacy and Safety of Topical Clascoterone Cream, 1%, for Treatment in Patients With Facial Acne: Two Phase 3 Randomized Clinical Trials. JAMA Dermatology. 2020.
https://jamanetwork.com/journals/jamadermatology/fullarticle/2765025
- Scopelliti MG, Kothare A, Karavitis M. A Novel 1726 Nm Laser System for Safe and Effective Treatment of Acne Vulgaris. Lasers in Medical Science. 2022.
https://doi.org/10.1007/s10103-022-03645-6
- Pulumati A, Jaalouk D, Algarin YA, et al. Targeting Sebaceous Glands: A Review of Selective Photothermolysis for Acne Vulgaris Treatment. Archives of Dermatological Research. 2024.
https://pubmed.ncbi.nlm.nih.gov/38850426/
- Alexiades M, Kothare A, Goldberg D, Dover JS. Novel 1726 Nm Laser Demonstrates Durable Therapeutic Outcomes and Tolerability for Moderate to Severe Acne Across Skin Types. Journal of the American Academy of Dermatology. 2023.
https://www.sciencedirect.com/science/article/pii/S0190962223010757
- Goldberg D, Ronan S, Bhatia A, et al. Safe and Effective Acne Treatment Across Skin Types With a 1726 Nm Sebum Selective Laser: One Year Data From a Prospective Multicenter Study. Journal of the American Academy of Dermatology. 2025.
https://www.sciencedirect.com/science/article/pii/S0190962225029007
- Kwon HH, Park HY, Choi SC, et al. Novel Device Based Acne Treatments: Comparison of a 1450 Nm Diode Laser and Microneedling Radiofrequency on Mild to Moderate Acne Vulgaris and Seborrhoea in Korean Patients Through a 20 Week Prospective, Randomized, Split Face Study. Journal of the European Academy of Dermatology and Venereology. 2018.
https://pubmed.ncbi.nlm.nih.gov/29178495/
- Ahn GR, Kim JM, Park SJ, Li K, Kim BJ. Selective Sebaceous Gland Electrothermolysis Using a Single Microneedle Radiofrequency Device for Acne Patients: A Prospective Randomized Controlled Study. Lasers in Surgery and Medicine. 2020.
https://pubmed.ncbi.nlm.nih.gov/31502662/
- Kim ST, Lee KH, Sim HJ, Suh KS, Jang MS. Treatment of Acne Vulgaris With Fractional Radiofrequency Microneedling. The Journal of Dermatology. 2014.
https://pubmed.ncbi.nlm.nih.gov/24807263/
- Manuskiatti W, Wongdama S, Viriyaskultorn N, et al. Long Term Efficacy and Safety of Nonablative Monopolar Radiofrequency in the Treatment of Moderate to Severe Acne Vulgaris. Lasers in Surgery and Medicine. 2024.
https://pubmed.ncbi.nlm.nih.gov/38221810/
- Manuskiatti W, Wongdama S, Li JB, et al. One Year Follow Up of Acne Vulgaris Patients Treated With Nonablative Monopolar Radiofrequency: Efficacy and Safety Assessment. Lasers in Surgery and Medicine. 2025.
https://pubmed.ncbi.nlm.nih.gov/40371601/
- Ishii L, Deoghare S, Boen M. Light and Laser Based Therapy in Treatment of Acne Vulgaris: A Clinical Review. Journal of the American Academy of Dermatology. 2025.
https://pubmed.ncbi.nlm.nih.gov/40550334/
- Jean Pierre P, Tordjman L, Ghodasara A, Nwosu C, Nouri K. Emerging Lasers and Light Based Therapies in the Management of Acne: A Review. Lasers in Medical Science. 2024.
https://doi.org/10.1007/s10103-024-04196-8