By Dr Gerard Ee
Introduction
GLP-1 medications have become one of the most discussed areas in modern medicine. In Singapore and around the world, many patients now search for terms such as GLP 1 for weight loss, Ozempic Singapore, Wegovy Singapore and Mounjaro Singapore because these medicines are strongly associated with diabetes care, appetite control and medically supervised weight management.
But in recent years, another question has become increasingly important: could GLP 1 for Alzheimer’s Disease become a future treatment direction?
Alzheimer’s disease remains one of the most challenging conditions in healthcare. Dementia affected around 57 million people worldwide in 2021, and Alzheimer’s disease is the most common form of dementia, contributing to about 60–70% of cases. Dementia affects memory, thinking, behaviour, daily independence and the wellbeing of caregivers, making it a major public health issue globally.
A recent phase 2b clinical trial, published in Nature Medicine, studied liraglutide, a GLP-1 receptor agonist, in people with mild to moderate Alzheimer’s disease. The study is important because it explored whether a drug class best known for diabetes and weight management might also influence brain metabolism, cognition and brain volume in Alzheimer’s disease.
The results were not a simple “yes” or “no”. Liraglutide did not significantly improve the study’s primary endpoint, which was cerebral glucose metabolism measured by FDG-PET. However, it did show encouraging signals in cognition and exploratory MRI brain-volume outcomes. This makes the study worth discussing carefully, especially now that semaglutide, the active ingredient in Ozempic and Wegovy, has recently failed to show a statistically significant reduction in Alzheimer’s disease progression in two large phase 3 trials.
For patients searching for Ozempic Singapore, Wegovy Singapore or Mounjaro Singapore, this distinction matters. These medicines are not interchangeable Alzheimer’s treatments, and the evidence for one GLP-1 medicine cannot automatically be applied to another.
What are GLP-1 medications?
GLP-1 stands for glucagon-like peptide-1. It is a naturally occurring hormone involved in blood sugar regulation, insulin release, appetite signalling and satiety. GLP-1 receptor agonists are medicines designed to mimic or enhance this pathway.
Traditionally, GLP-1 medications were used mainly for type 2 diabetes. More recently, they have become widely known for medically supervised weight management. This is why GLP 1 for weight loss has become such a common search term.

In Singapore, several GLP-1 or incretin-based medicines are relevant to this conversation. Ozempic Singapore refers to semaglutide, which HSA listed in April 2021 for adults with insufficiently controlled type 2 diabetes mellitus as an adjunct to diet and exercise. Wegovy Singapore refers to semaglutide for weight management; HSA listed Wegovy in March 2023 as an adjunct to a reduced-calorie diet and increased physical activity for weight management in adults with obesity or overweight with at least one weight-related comorbidity. Some patients misspell this as Wegrovy Singapore, but the correct brand name is Wegovy.
Mounjaro Singapore refers to tirzepatide. Tirzepatide is not simply a GLP-1 receptor agonist; it is a dual incretin medication acting on GIP and GLP-1 pathways. HSA listed Mounjaro in March 2023 for glycaemic control in adults with type 2 diabetes, and a June 2025 HSA announcement also listed Mounjaro for weight management in adults meeting BMI and comorbidity criteria.
These distinctions are important. Liraglutide, semaglutide and tirzepatide are related, but they are not the same drug. They differ in structure, dose, duration of action, clinical indications and available evidence.
Why are GLP-1 medicines being studied in Alzheimer’s disease?
Alzheimer’s disease is complex. It is not caused by one single pathway. It involves amyloid-beta accumulation, tau aggregation, neuroinflammation, glial activation, synaptic dysfunction and progressive neurodegeneration. The Nature Medicine paper explains that because Alzheimer’s disease involves multiple biological processes, treatments that influence several targets may be useful to study.
This is where GLP 1 for Alzheimer’s Disease becomes scientifically interesting.
Liraglutide has shown neuroprotective effects in animal models. In preclinical Alzheimer’s models, liraglutide has been associated with improvements in memory, reduced synaptic loss, reduced beta-amyloid and tau aggregation, lower neuroinflammation, reduced oxidative stress and improved insulin signalling.
These findings do not prove that liraglutide treats Alzheimer’s disease in humans. Animal models are useful for generating scientific hypotheses, but human clinical trials are needed to test whether the same effects translate into meaningful patient benefits.
That is what the ELAD trial attempted to do.
The ELAD trial: a summary of the paper
The study was called Evaluating Liraglutide in Alzheimer’s Disease, or ELAD. It was a multicentre, randomised, double-blind, placebo-controlled phase 2b trial involving 204 participants with mild to moderate Alzheimer’s disease syndrome and no diabetes. Participants were randomly assigned to receive liraglutide or placebo for 52 weeks.
The study was designed to evaluate whether liraglutide could affect brain glucose metabolism, cognition, MRI brain volume and safety in people with Alzheimer’s disease.
Participants received once-daily subcutaneous injections. The liraglutide dose started at 0.6 mg once daily and was escalated to 1.8 mg within four weeks if tolerated. Those who did not tolerate 1.8 mg could remain temporarily at 1.2 mg before further attempts at dose escalation.
This is worth noting because the liraglutide dose used in ELAD was closer to the diabetes-dose range, not the higher liraglutide dose used for obesity under the Saxenda brand in some countries. Therefore, this trial should not be interpreted as a GLP 1 for weight loss trial. It was an Alzheimer’s disease trial using a GLP-1 receptor agonist.
Key trial results
| Trial feature | Result |
|---|---|
| Study name | ELAD: Evaluating Liraglutide in Alzheimer’s Disease |
| Trial type | Multicentre, randomised, double-blind, placebo-controlled phase 2b trial |
| Participants | 204 people with mild to moderate Alzheimer’s disease syndrome and no diabetes |
| Treatment | Liraglutide once daily vs placebo |
| Duration | 52 weeks |
| Primary endpoint | Change in cerebral glucose metabolism measured by FDG-PET |
| Primary result | No significant difference between liraglutide and placebo |
| Cognitive result | ADAS-Exec score performed better in liraglutide-treated participants |
| Functional/global measures | No significant difference in ADCS-ADL or CDR-Sum of Boxes |
| MRI findings | Exploratory analyses showed lower reductions in temporal lobe and total grey matter volume |
| Safety | Generally safe and well tolerated; gastrointestinal side effects were most common |
The primary outcome was negative. The study found no significant difference in cerebral glucose metabolism between the liraglutide and placebo groups. The reported adjusted difference was −0.17, with a 95% confidence interval from −0.39 to 0.06 and a P value of 0.14.
This is the most important result. A responsible article cannot claim that liraglutide has been proven to treat Alzheimer’s disease. It has not. The trial did not meet its primary endpoint.
However, the cognitive result was more encouraging. The secondary outcome of ADAS-Exec, a cognitive measure combining the Alzheimer’s Disease Assessment Scale-Cognitive Subscale and executive-domain testing, performed better in the liraglutide group than the placebo group. The reported difference was 0.15, with a 95% confidence interval of 0.03 to 0.28 and an unadjusted P value of 0.01.
At the same time, other clinically important measures did not show significant differences. The study found no significant difference in ADCS-ADL, which assesses activities of daily living, or CDR-Sum of Boxes, a global measure commonly used in Alzheimer’s disease trials.
This means the cognitive signal is interesting, but not enough on its own to establish liraglutide as an Alzheimer’s treatment.
MRI brain-volume findings
One of the most interesting parts of the ELAD trial was the MRI analysis. The study did not find significant treatment differences in hippocampal volume, entorhinal cortex volume or ventricular volume. However, exploratory analyses showed lower reductions in temporal lobe volume and total grey matter volume among liraglutide-treated participants compared with placebo.
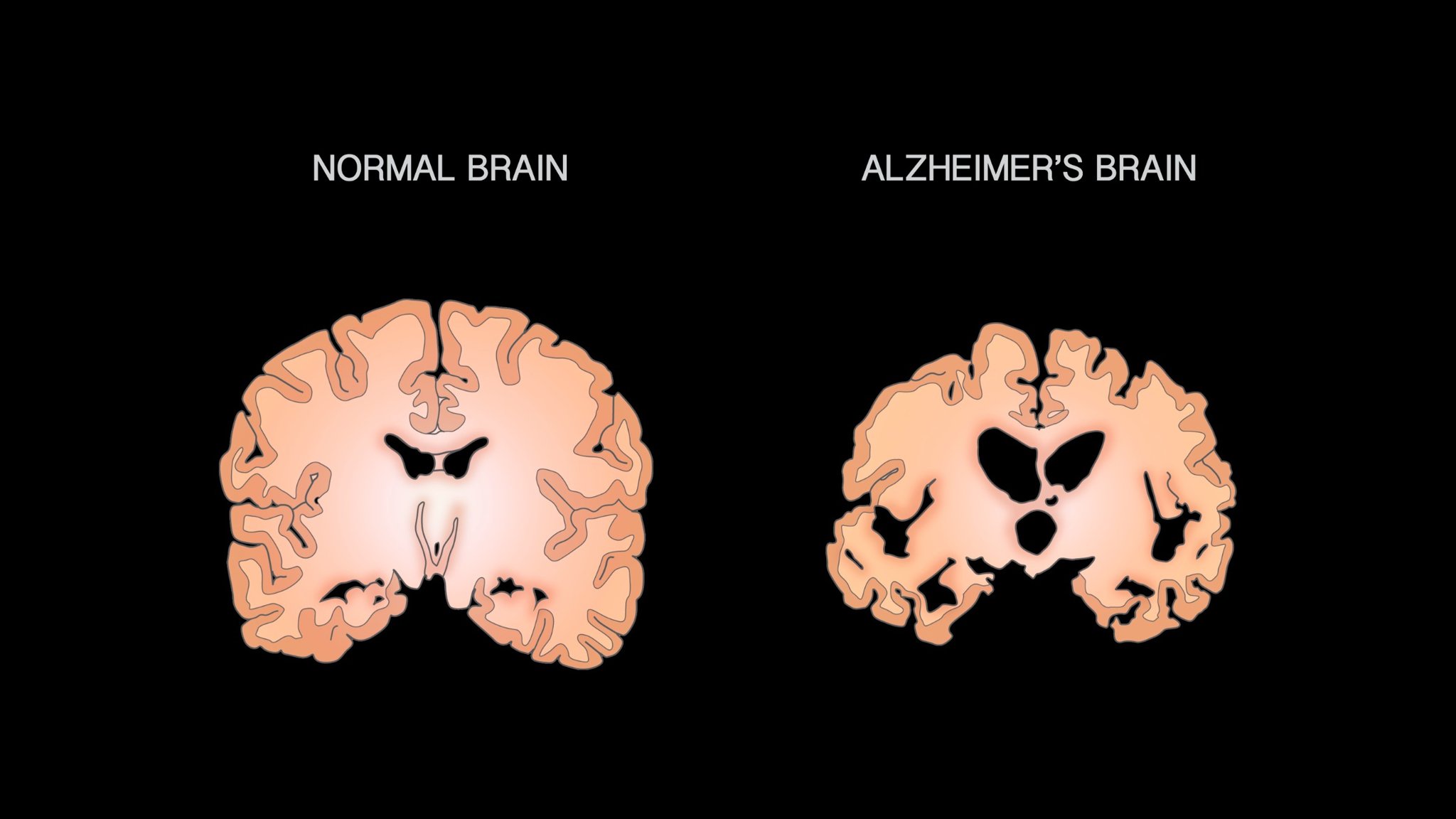
The reported difference in temporal lobe volume reduction was 696 mm³, while the difference in total grey matter volume reduction was 7,274 mm³. Parietal and frontoparietal regions also showed trends toward lower volume loss.
This matters because brain atrophy is part of Alzheimer’s disease progression. If a therapy can slow brain-volume loss, it may suggest a possible neuroprotective effect. However, this finding was exploratory and should be interpreted cautiously.
The authors themselves stated that the cognitive and MRI findings need confirmation in larger studies.
Safety and tolerability
Liraglutide was generally safe and well tolerated in the ELAD trial. The study reported 991 adverse events over 12 months: 541 in the liraglutide group and 450 in the placebo group. Serious adverse events occurred in 7 participants in the liraglutide group and 18 participants in the placebo group, with most serious events considered unlikely to be related to the study treatment.
The most common adverse events were gastrointestinal. These included nausea, bloating, diarrhoea, dyspepsia, anorexia and weight loss. Up to 5% weight loss occurred in 39.2% of patients in the liraglutide arm compared with 12.6% in the placebo arm. Weight loss of 5–10% occurred in 8.9% of patients in the liraglutide group compared with 1.1% in the placebo group.
This is where the overlap between GLP 1 for Alzheimer’s Disease and GLP 1 for weight loss becomes clinically important. In some patients, weight loss may be beneficial, especially where obesity, insulin resistance or metabolic syndrome are present. But in older or frail patients, unintended weight loss can be a concern.
For Alzheimer’s disease, preserving nutrition, muscle mass and strength is important. A medicine that reduces appetite may require careful monitoring in older adults, especially if they are already losing weight.
Why semaglutide matters: Ozempic Singapore and Wegovy Singapore
The reason it is valid to mention Ozempic Singapore and Wegovy Singapore in an article about Alzheimer’s disease is that both are semaglutide products, and semaglutide has now been tested in large Alzheimer’s disease trials.
Novo Nordisk announced in November 2025 that the EVOKE and EVOKE+ phase 3 trials did not demonstrate a statistically significant reduction in Alzheimer’s disease progression with oral semaglutide compared with placebo. These trials enrolled 3,808 adults with early-stage symptomatic Alzheimer’s disease and measured disease progression using CDR-Sum of Boxes.
This is a major point for patients reading about GLP-1 medications. Semaglutide is the active ingredient in Ozempic, used for type 2 diabetes, and Wegovy, used for chronic weight management. Novo Nordisk also states that semaglutide is marketed as Ozempic and Rybelsus for type 2 diabetes, and Wegovy for chronic weight management.
For people searching Ozempic Singapore or Wegovy Singapore, the message is clear: semaglutide remains important in diabetes and weight management, but the available Alzheimer’s disease trial results do not show that semaglutide slows clinical progression of Alzheimer’s disease.
This does not mean semaglutide has no brain-related biological effects. Novo Nordisk reported improvements in some Alzheimer’s disease-related biomarkers, but these did not translate into delayed disease progression in EVOKE and EVOKE+.
Did liraglutide perform better than semaglutide in Alzheimer’s disease?
This is a tempting question, but it needs a careful answer.
The liraglutide ELAD trial and the semaglutide EVOKE trials were not head-to-head studies. They used different drugs, different formulations, different trial phases, different durations, different populations and different endpoints. Therefore, we cannot say that liraglutide is definitively “better” than semaglutide for Alzheimer’s disease.
However, we can say that the clinical signals differed.
Liraglutide did not meet its primary FDG-PET endpoint, but it showed an encouraging signal on ADAS-Exec cognition and exploratory MRI brain-volume outcomes. Semaglutide, on the other hand, was tested in two large phase 3 Alzheimer’s trials and did not show a statistically significant reduction in disease progression compared with placebo, despite biomarker improvements.
This difference gives a scientifically valid reason to discuss Ozempic and Wegovy in the same article as liraglutide. Patients may assume that all GLP-1 medications behave the same way, but Alzheimer’s disease research suggests the story is more complicated.
A cautious interpretation is this: GLP 1 for Alzheimer’s Disease remains an active research area, but the evidence is not strong enough to recommend GLP-1 medications as Alzheimer’s treatment.
Where does Mounjaro Singapore fit in?
Mounjaro Singapore is also relevant because many patients now group Ozempic, Wegovy and Mounjaro together when asking about injectable weight-loss medications. However, Mounjaro is tirzepatide, a dual incretin medicine, not the same as liraglutide or semaglutide.
In Singapore, HSA listed Mounjaro for type 2 diabetes in March 2023, and a later HSA announcement in June 2025 listed Mounjaro for weight management in adults who meet BMI and comorbidity criteria.
At present, the liraglutide Alzheimer’s trial should not be used as evidence that Mounjaro treats Alzheimer’s disease. The same applies to Ozempic and Wegovy. These medicines may be relevant to weight, insulin resistance and metabolic health, but Alzheimer’s disease treatment requires direct evidence from Alzheimer’s trials.
This is especially important in a Singapore clinical setting, where patients may come in asking whether Mounjaro Singapore, Ozempic Singapore or Wegovy Singapore can protect the brain. The honest answer is that metabolic health and brain health are connected, but no GLP-1 or incretin-based medicine should currently be presented as an approved Alzheimer’s treatment.
GLP 1 for weight loss and brain health: what patients should understand
There is a reasonable biological link between metabolic health and brain health. The WHO lists high blood pressure, high blood sugar, being overweight or obese, smoking, physical inactivity and social isolation among risk factors associated with dementia risk.
This does not mean weight-loss medications prevent Alzheimer’s disease. It means that improving metabolic health may be one part of a broader long-term brain-health strategy.
For patients exploring GLP 1 for weight loss, the main proven benefits still relate to approved indications such as type 2 diabetes, obesity and weight management, depending on the specific medicine and local regulatory approval. In Singapore, HSA indications for Ozempic, Wegovy and Mounjaro are focused on diabetes and/or weight management, not Alzheimer’s disease.
A good clinical conversation should separate three ideas:
First, GLP-1 medicines can be useful for diabetes and weight management in appropriate patients. Second, better metabolic health may support healthier ageing. Third, using GLP-1 medicines as treatment for Alzheimer’s disease is still investigational.
That distinction protects patients from hype while still acknowledging the exciting science.
What this paper proves — and what it does not prove
The ELAD paper proves that liraglutide can be studied safely in non-diabetic patients with mild to moderate Alzheimer’s disease over 52 weeks. It also shows that liraglutide produced an encouraging signal in one cognitive measure and exploratory MRI brain-volume outcomes.
But the paper does not prove that liraglutide treats Alzheimer’s disease. It did not meet its primary endpoint. It did not show significant benefit in activities of daily living or CDR-Sum of Boxes. The secondary and exploratory findings were not corrected for multiple comparisons, and the authors stated that the results need confirmation in larger studies.
It also does not prove that Ozempic, Wegovy or Mounjaro help Alzheimer’s disease. In fact, semaglutide’s EVOKE and EVOKE+ results show why we must be cautious: a medication may improve some biomarkers without improving clinical disease progression.
Practical takeaway for Singapore patients
For patients searching Ozempic Singapore, Wegovy Singapore, Wegrovy Singapore or Mounjaro Singapore, the most practical message is this:
These medicines are important developments in diabetes and weight management. They may help suitable patients lose weight, improve glycaemic control and manage metabolic risk under medical supervision. But they are not approved Alzheimer’s treatments, and they should not be used with the expectation that they will slow or reverse Alzheimer’s disease.
For patients and families affected by Alzheimer’s disease, the liraglutide trial is encouraging but early. It supports further research into GLP 1 for Alzheimer’s Disease, especially larger trials with stronger biomarker selection, longer follow-up and clearer clinical endpoints.
For patients considering GLP 1 for weight loss, the focus should remain on appropriate medical assessment, careful dosing, monitoring of side effects, nutrition, muscle preservation and long-term lifestyle support.
Conclusion
The ELAD trial is an important study because it expands the conversation around Alzheimer’s disease. Instead of looking only at amyloid or tau, it explores whether metabolic and inflammatory pathways may also be useful treatment targets.
Liraglutide did not meet the study’s primary endpoint, so it cannot be called a proven Alzheimer’s treatment. However, its cognitive and MRI signals make it a meaningful study that deserves attention.
The semaglutide story is also important. Although semaglutide is widely known through Ozempic Singapore and Wegovy Singapore, the EVOKE and EVOKE+ trials did not show a statistically significant slowing of Alzheimer’s disease progression. This contrast helps patients understand that not all GLP-1 medications should be viewed as the same, especially when discussing brain health.
Mounjaro Singapore adds another layer to the conversation because tirzepatide is now part of the weight-management discussion, but it should not be assumed to have Alzheimer’s benefits without direct clinical evidence.
The balanced conclusion is this: GLP 1 for Alzheimer’s Disease is promising but unproven. GLP 1 for weight loss is already clinically relevant for suitable patients, but its role in Alzheimer’s prevention or treatment remains investigational.
As research continues, patients should avoid hype and seek personalised medical advice. The future of Alzheimer’s care may involve multiple approaches — metabolic health, vascular risk reduction, inflammation, lifestyle, biomarkers and disease-modifying therapies — but for now, GLP-1 medicines should be used for their approved indications, not as Alzheimer’s treatment.
References
- Edison P, Femminella GD, Ritchie C, et al. Liraglutide in mild to moderate Alzheimer’s disease: a phase 2b clinical trial. Nature Medicine. Published 1 December 2025; Nature Medicine volume 32, pages 353–361, 2026.
- World Health Organization. Dementia fact sheet. Updated 31 March 2025.
- Health Sciences Authority Singapore. New drug approvals — April 2021: Ozempic, semaglutide.
- Health Sciences Authority Singapore. New drug approvals — March 2023: Wegovy, semaglutide; Mounjaro, tirzepatide.
- Health Sciences Authority Singapore. New drug approvals — June 2025: Mounjaro weight management indication.
- Novo Nordisk. EVOKE phase 3 trials did not demonstrate a statistically significant reduction in Alzheimer’s disease progression. Published 24 November 2025







